Homocysteine is a natural compound in the body. It is often linked with an increased risk of heart disease. High concentrations are seen as bad, but does that mean all homocysteine is harmful? Not exactly!
This article explores what homocysteine is. We’ll also look at how its measurement can give you insights into health, including your methylation cycle. Learn more about how homocysteine affects the body and how a simple blood test could give you some valuable insights.
What is Homocysteine?

Homocysteine is an amino acid created in the body as a result of methylation. This conversion reaction happens when SAMe donates its methyl group to a methyltransferase enzyme. This transfer allows these compounds to do the jobs they were designed to do.
Methylation cannot occur without making homocysteine.

Methionine and homocysteine are both amino acids. They have the same molecular structure except for one difference:
- Methionine contains a methyl group
- Homocysteine does not contain a methyl group
Similarly, they are both necessary for making other compounds. Methionine is required to make SAMe. As part of the methylation cycle, homocysteine either helps make more SAMe, or it can go a different direction to make glutathione.
Is Homocysteine Bad?

Homocysteine is often seen as a negative compound. But it’s the amount of homocysteine that determines whether it is helpful or harmful.
High levels of homocysteine are referred to as hyperhomocysteinemia. High homocysteine is a risk factor for medical conditions like heart problems, atherosclerosis, cognitive problems, thrombosis (blood clots), and more. (1) This is because it leads to the impairment of nitric oxide. This affects the blood vessels by causing poor blood flow. (2)
Homocysteine levels that are balanced are useful and supportive of healthy methylation. It can be recycled into methionine by two different routes via:
- MTR
- BHMT
This recycling of homocysteine can support healthy levels of SAMe and an overall balanced methylation cycle.
Homocysteine can also be processed by the cystathionine-B-synthase (CBS) enzyme to make glutathione. Glutathione has significant antioxidant activity in the body.
Homocysteine is necessary for methionine, SAMe, healthy methylation, and glutathione. While high homocysteine levels can be harmful, not having enough homocysteine can interfere with all of those conversion processes. Low homocysteine is called hypohomocysteinemia.
When it comes to homocysteine, balance is key. Too much or too little are both problems for optimal health.
You can have homocysteine problems for several reasons:
- Lifestyle and environment: not enough nutrients that support the methylation cycle (active B12, active folate), a diet that is high in processed foods, low levels of exercise
- Genetic SNPs (variants): Mutations in certain genes like CBS, MTHFR, MTR, and MTRR can cause a condition known as homocystinuria. This can lead to excessive homocysteine or problems converting homocysteine into other compounds. (3)
- Both lifestyle and genetic SNPs: Many people are not aware that they have genes contributing to elevated homocysteine, and doctors do not routinely test for this. If your lifestyle contributes to high homocysteine and you already have a genetic predisposition to problems with homocysteine conversion, you have a high risk of homocysteine-related problems.
Anything that interferes with your body’s ability to convert homocysteine for needed purposes can influence your health in major ways.
Problems with Low Homocysteine
Low levels of homocysteine can also be a problem. Your body needs homocysteine so that your CBS enzyme can convert it into cystathionine. After that, it gets converted to cysteine. It goes through yet another conversion to become glutathione in the liver. Without glutathione, the liver will be unable to normally perform its vital detoxification functions.
Homocysteine levels lower than 7 μmol/L in adults can indicate that there is not enough homocysteine for normal glutathione production.
Problems with High Homocysteine

High homocysteine is more common and problematic in a different way. Elevated homocysteine levels can lead to the build-up of a molecule called S-Adenosyl Homocysteine (SAH). SAH slows down the function of important methyltransferases (MT).
MTs are enzymes like catechol-o-methyltransferase (COMT) and histamine-n-methyltransferase (HNMT). COMT and HNMT are needed to metabolize estrogen and cortisol and break down histamine. (4) If homocysteine gets high, you may also experience hormone imbalances from too much estrogen and too much cortisol. You could also experience more signs of histamine intolerance as your body struggles to properly resolve histamine. If you already have an impaired DAO gene, your histamine issues could be even worse.
Homocysteine is formed when SAMe, an important methyl donor, gives its methyl group to one of the following enzymes:
- GAMT to make creatine
- PEMT to make phospholipids
- COMT to metabolize estrogen
- HNMT to eliminate histamine
- PNMT to make epinephrine/adrenalin
- ASMT to make melatonin
Because of this methyl group donation, SAMe becomes SAH. The Adenosylhomocysteinase enzyme (AHCY) then converts SAH into homocysteine by taking away the adenosine molecule.
From there, homocysteine is either re-methylated back into SAMe (making a complete loop), or it is used to make glutathione.
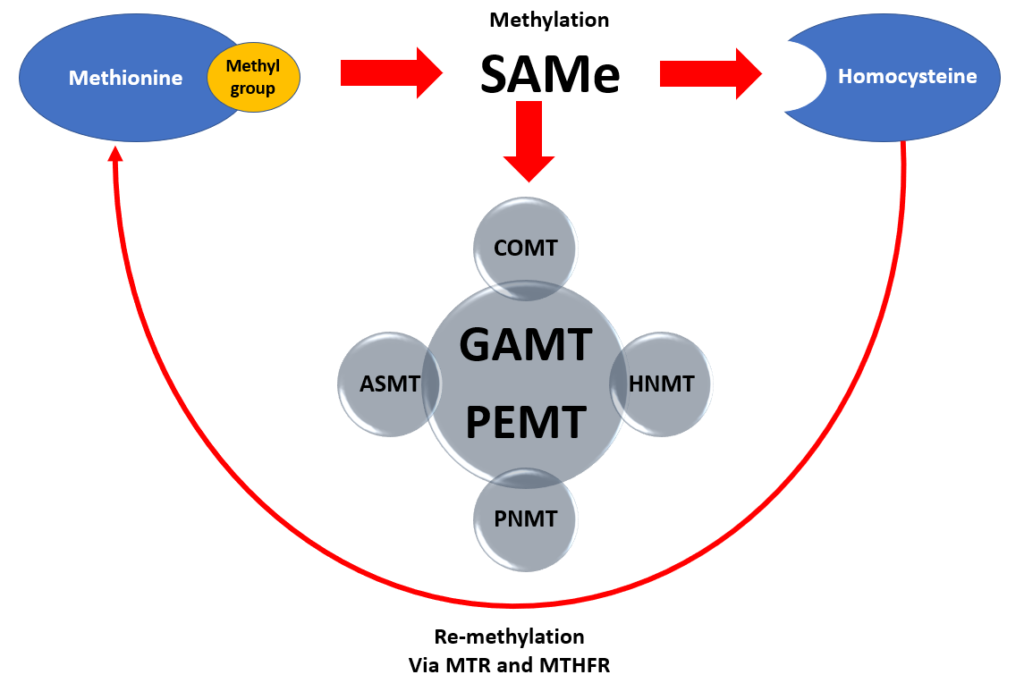
But if your body cannot effectively convert homocysteine into SAMe or glutathione, then your homocysteine levels get too high. This can happen because of slowed function with MTHFR, MTR, or CBS enzymes.
If homocysteine levels continue to accumulate, it gets converted into SAH. This triggers a string of methylation problems, such as:
- Reduced creatine levels
- Reduce phospholipids
- Decreased breakdown of estrogen
- Higher histamine levels
- Decreased epinephrine production
- Lowered melatonin levels
As a result, you may have a whole host of symptoms:
- Fatigue
- Estrogen dominance and hormone problems
- Sensitivities
- Poor sleep
- Muscle problems
- Digestion issues
High homocysteine is also used as a biomarker for some nutrient problems and can be a sign of:
- Folate deficiency
- Vitamin B12 deficiency
- Vitamin B6 deficiency
These three nutrients are needed to support homocysteine metabolism and stop homocysteine from accumulating. (5) If these levels are low, they can be supported with vitamin supplementation. Hyperhomocysteinemia can also occur if you have mutations in genes involved with homocysteine metabolism. These include:
Healthcare providers have different ranges for what is considered high homocysteine, but anything over 15 μmol/L is considered to be high. Some providers will use a narrower range and may consider anything above 9-10 to be too high. Your healthcare provider will let you know if your homocysteine is in range or not.
Symptoms of Homocysteine Dysfunction
Some of the symptoms of high and low homocysteine can often be similar. You cannot tell whether your homocysteine is elevated based on symptoms alone. If high homocysteine is due to a slower CBS enzyme, it can have the same effect on your CBS cycle as low homocysteine. Both high and low homocysteine can cause symptoms like:
- Pale skin
- Weakness
- Fatigue
- Poor exercise tolerance
- Dizziness
- Sores in the mouth or tongue>
- Tingling sensation in the feet
- Detoxification problems
- Thyroid dysfunction
- Increased sensitivities
- Skin conditions
- PMS or mood issues
- Poor sleep

How Do You Measure Homocysteine?

You can learn what your levels of homocysteine are from a simple blood test. The homocysteine test measures plasma homocysteine levels. A healthcare provider can order this. The results will be listed as total homocysteine and may range from 5 to well over 15 μmol/L. Providers may have different ranges that they want to see, depending on your health. Most ranges consider anything over 15 μmol/L (micromoles per liter) to be elevated.
An optimal range is typically considered to be 7-9 μmol/L.
Certain medical conditions may warrant closer management of homocysteine. High levels of homocysteine can contribute to risk factors for heart problems, vascular problems, blood pressure issues, cholesterol problems, bone health problems, cognitive disorders, and more. (10,11,12,13)
Nutrients for Homocysteine Balance

Maintaining healthy homocysteine levels may require nutrient support or vitamin supplementation. This can include:†
- Folate (not folic acid) in active forms like L-5-MTHF or folinic acid
- Vitamin B12 in active forms like methylcobalamin, adenosylcobalamin, or hydroxocobalamin
- Vitamin B6 in its active form (pyridoxal 5’ phosphate)
These nutrients support the conversion of homocysteine into methionine or glutathione, and may support healthy homocysteine levels if they are too high.
How to Support Healthy Homocysteine
There are many things that you can do to support healthy homocysteine balance in the body.†
- Support your MTR enzyme with dietary zinc, vitamin B12, and folate.
- Support healthy CBS enzyme function with vitamin B6 or pyridoxal-5-phosphate.
- Keep your methylation cycle working optimally with active B12, folate, and B6.
The Bottom Line
Homocysteine is not good or bad. Like most things, it has a purpose but needs to remain in balance. The amount of homocysteine determines whether it’s helpful or harmful. Balanced homocysteine levels are supportive of healthy methylation. Homocysteine that is too high or too low can provide insight into how well your methylation cycle is working. An optimal homocysteine range is typically considered to be 7-9 μmol/L. Homocysteine levels lower than 7 μmol/L in adults can indicate that there is not enough homocysteine for normal glutathione production. While healthcare providers differ in what they consider to be elevated, anything over 15 μmol/L is generally considered as high homocysteine levels. Some providers consider anything above 9-10 to be too high. Your healthcare provider can order a test to measure your total homocysteine levels. Once you know what yours are, you now know what genes, nutrients, and lifestyle behaviors are involved in disrupting or providing balance.
References
- https://journals.sagepub.com/doi/full/10.1177/1179573520962230
- https://nutritionj.biomedcentral.com/articles/10.1186/1475-2891-14-6
- https://medlineplus.gov/genetics/condition/homocystinuria/
- https://pubs.acs.org/doi/10.1021/acschembio.5b00812
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6877406/
- https://www.ahajournals.org/doi/10.1161/01.cir.0000165142.37711.e7
- https://pubmed.ncbi.nlm.nih.gov/15890029/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2628129/
- https://www.sciencedirect.com/science/article/pii/S0969212602007967
- https://www.ahajournals.org/doi/10.1161/01.hyp.0000101690.58391.13
- https://pubmed.ncbi.nlm.nih.gov/16724071/
- https://pubmed.ncbi.nlm.nih.gov/12530932/
- https://www.researchgate.net/publication/7568439_Homocysteine_-_A_newly_recognised_risk_factor_for_osteoporosis










